Rutland First Aid Training
Learn essential first aid skills
First Aid Training in Rutland, Leicestershire, Lincolnshire, Cambridgeshire
(covering towns such as Grantham, Melton Mowbray, Oakham & Stamford)
RUTLAND FIRST AID
At Rutland First Aid Training, we pride ourselves on providing a comprehensive range of first aid courses to cater to diverse requirements to Leicestershire, Lincolnshire, Rutland & Cambridgeshire, covering towns: Oakham, Grantham, Melton Mowbray, Stamford and the surrounding areas. Whether you are a parent, grandparent, nanny, work with children, or represent a business that has a legal obligation to ensure first aid preparedness, we have got you covered.
Our onsite and offsite first aid training courses are designed to equip you with the knowledge and skills needed to respond confidently and efficiently in case of a medical emergency. We understand that potentially every individual and companies needs differ, and that's why we have developed a range of courses that cater to different requirements.
For those who are new to first aid, we offer first aid courses that cover the basics of administering first aid in different situations. Parents and grandparents can enroll in courses that specifically focus on first aid for children. Nannies and childcare professionals can also benefit from our paediatric first aid courses.
Businesses have a legal obligation to ensure the safety of their employees so opt for our workplace first aid courses. Our courses are tailored to specific industries and are designed to help employees respond effectively in case of a medical emergency. If you can't find the course you are looking for or have a question, please do not hesitate to get in touch with us. Our team of experts is always ready to discuss your requirements.
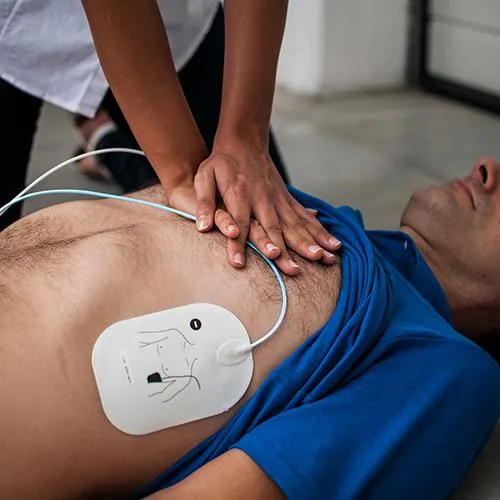
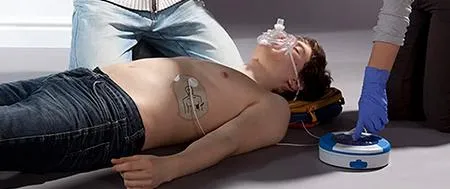
AED & CPR
The CPR & AED course offers individuals the chance to acquire life-saving skills that can make a significant difference in emergency situations to potentially save lives.
EMERGENCY FIRST AID AT WORK
The Emergency First Aid at Work course is a one-day intensive first aid program to ensure that your workplace meets Health & Safety requirements to provide First Aid quickly and confidently.
FIRST AID AT WORK
The First Aid At Work Course ensures your staff are trained with the necessary skills to handle workplace medical emergencies by enrolling this 3-day First Aid at Work course.
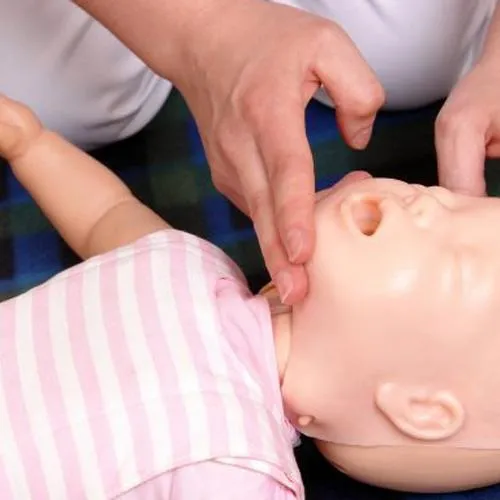
CARE FOR CHILDREN
The Care For Children two-day (12hr) course provides the necessary training to give children care in and meets EYFS, Ofsted, CSSIW and Scottish Early Years standards.
Paediatric First Aid | Workplace First Aid | Lay Person First Aid
WHY CHOOSE RUTLAND FIRST AID
Industry Recognised
Our courses are recognised by HSE, Ofsted and follow ILCOR guidelines.
On-Site Training
We can deliver tailor-made courses at your workplace, and at a price that meets your budget.
CUSTOM QUOTES
Need a custom training quote? No problem. Just send us an email with your requirements.
Flexible Dates
Although we offer training dates for specific courses, We can arrange training courses around you.
Group Discounts
Do you have 4 or more people who need training? We can offer discounts for groups.
First Aid Equipment
Need a defibrillator (AED) or HSE Approved First Aid Kits? No problem. Contact us for more!
Check out our most popular products
Select your FIRST AID PATH
First Aid TRAINING in Rutland
Established in the growing rural county of Rutland, it became clear that new and expanding businesses had an urgent need for first aid training. Responding to this demand, Rutland First Aid Training was born. At Rutland First Aid Training, we provide tailored first aid training solutions to suit a range of needs - from the everyday parent looking for peace of mind to experienced professionals. Our courses recognise these varying requirements and offer an in-depth overview with crucial information needed by those who have legal duties regarding first aid regulations.
Our courses are designed to get you the most out of your First Aid training, which is why they only come in small sizes. No more than four persons and no less than two on any open course! With our expert team ready to answer any questions throughout, we want everyone who attends one of our classes with us to gain life-saving skills that can give them the confidence they need should an emergency arise. Get in touch today for all your first aid needs.
ABOUT US
With interactive and realistic training devices, our aids give users the opportunity to practice lifesaving skills like helping someone who is choking. So you can confidently face any emergency situation in real life!
QUALITY HANDS ON TIME
Our courses are designed to provide superior quality training; perfect for those looking to gain critical, life-saving skills. You'll have plenty of time with our experienced instructors to find the confidence to care.
GUIDANCE FOR EMPLOYERS
We help employers assess their first-aid needs based on a range of factors, such as workplace hazards and size. This process, helps them determine the necessary first aid personnel to ensure worker safety.
BESPOKE TRAINING
Our courses are tailored to suit your needs, and we don't limit ourselves! Travelling across the Midlands in Leicester, Melton Mowbray, Peterborough and Stamford ensuring our services reach far beyond one city.
Hear what our first aid students have to say...
TESTIMONIALS
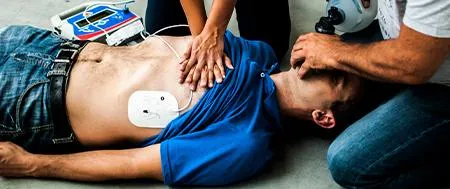

A really good training course, very professionally presented by Tracy. I’ve been on lots of training courses over the years and too often they can be soporific! Tracy is one of those rare training professionals who can deliver training and keep a person interested all day! Great course. Highly recommended!

Alan Eager
Google Review
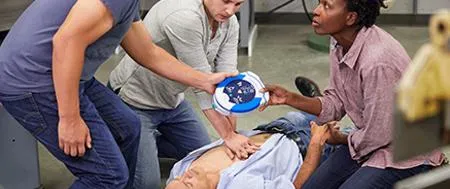

Rutland first aid are professional yet kept the courses fun and interactive and use some very interesting props. As a driving instructor I wanted to be able to deal with any issues with my students but also any issues I may come across on the roads. Highly recommended.

James Dames
Google Review

Couldn't recommend Tracy and her team enough for a first aid course. Having to renew it every 3 years used to send me to sleep. Not with these guys! Professional, up to date and with lots of toys to play with, without the death by powerpoint.

Mike Gould
Google Review

Here at Rutland First Aid Training we strive to provide high quality, personalised, fun and informative first aid courses.
Our courses are recognised by HSE, Ofsted and follow ILCOR guidelines.
Short Cuts
Find what you are looking for:
Dental CPD Courses
Get In Touch
If you have any questions or would like to discuss your requirements in further detail, our team are always happy to assist you.
1 Old Station Yard, Whissendine Road, Ashwell, Rutland LE15 7SP
@ 2025 Copyright Rutland First Aid Training. All rights reserved.
Rutland First Aid Training is a trading name of Dive Rutland Limited. Company No: 9433835.